Antenatal care is the attention mothers receive during pregnancy. It ensures you and your baby are in the best state of health. Over the period of pregnancy, the doctor follows up on you and your baby’s health to ensure your pregnancy goes as smoothly as possible.
Attending your antenatal appointments is quite important. Any potential risks to the baby can be identified and prevented or reduced. Antenatal care is important in the prevention of several pregnancy complications such as preeclampsia.
Antenatal clinics serve as good avenues to learn more about the baby’s growth per trimester. This is a chance for the doctors and midwives to educate you on any important changes in your lifestyle you may need to make.
Some hospitals have classes just before the clinics begin. Others have these on special days. Here, you will get information that will prepare you for childbirth, care of your baby such as bathing, diapering, breastfeeding.
What happens during the antenatal clinic?

The antenatal care you get throughout your pregnancy depends on:
- your health and any risks you or your baby may have
- the stage of pregnancy you are at, and
- any problems you may experience.
The caregiver would :
- Ask for the date of your last period, to estimate when the baby is due, what trimester you are in and what this means for you and your baby(ies)
- Find out about your medical history, general health, and how any previous pregnancies were
- Ask for the ethnic origins of you and your partner to find out whether your baby may be at risk of certain genetic inherited conditions
- Confirm what (if any) medication you may be taking
- Ensure you’ve had a recent pap smear (to assess the risk of cervical cancer)
- Make sure you are in a good state of mental health, and providing support if you have depression or anxiety
- Check your blood pressure and weight
- Test your urine
- Provide advice on a healthy diet
- Examine your tummy to determine if you have a singleton or multiple pregnancy
- Estimate the baby’s position and size, and listen to the baby’s heartbeat
- Advise you on care for your baby after pregnancy
How many antenatal visits will I have?
The frequency of your antenatal visits is determined by the results of your assessments. Pregnancies with possible complications would come with more antenatal visits, for example, if a mother has gestational diabetes or sickle cell disease, the doctor needs to monitor the pregnancy more closely than others.
In most hospitals in Nigeria, they schedule you to have one visit per month until the pregnancy is about 22 weeks. Then one visit every two weeks till about 32 weeks and once a week till birth.
What assessments would I undergo?

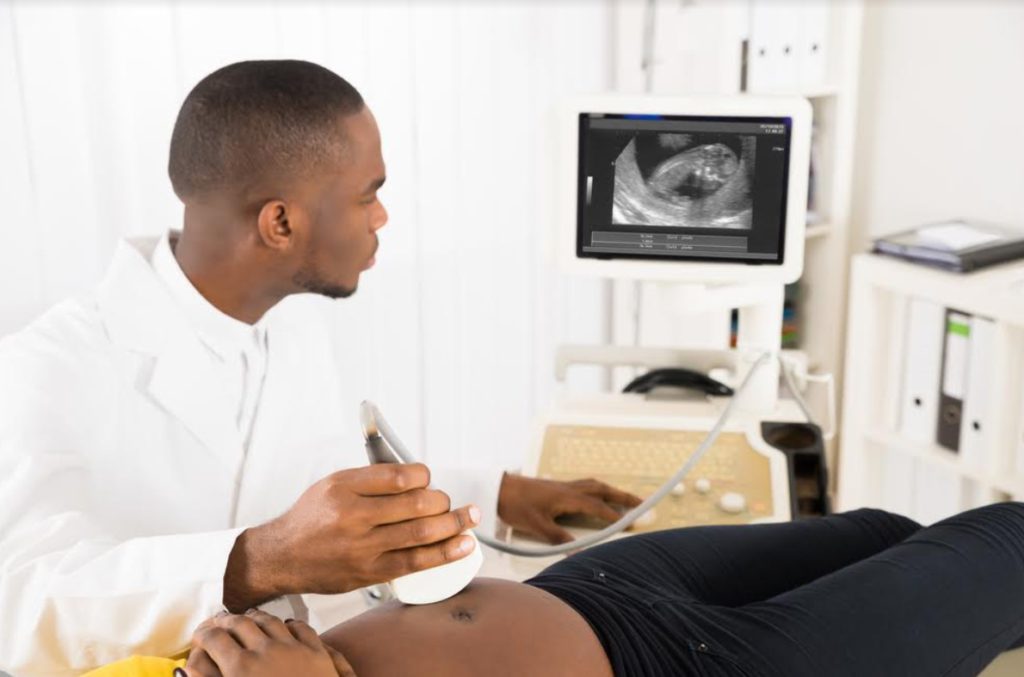
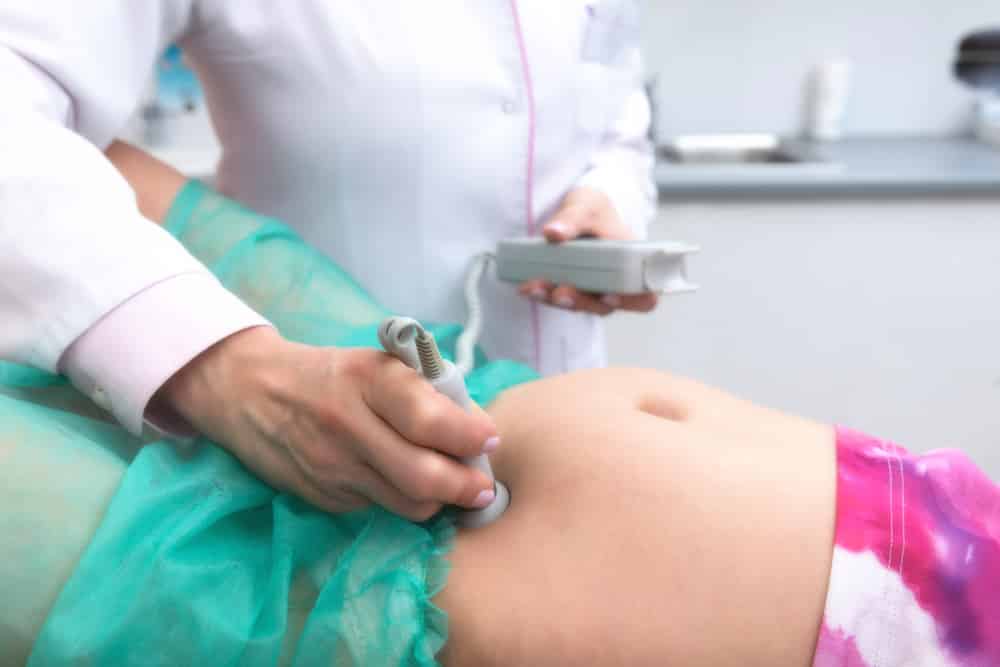
You would have ultrasound pregnancy scans done between 8 to 14 weeks to check for any abnormalities in the baby’s organs. These are repeated based on need.
Also, you would have blood tests to check for your blood group and genotype, HIV, hepatitis B and syphilis, and other infections that can affect your pregnancy or be passed on to your baby. Every visit, your doctor would also examine your pregnancy to check the baby’s heartbeats and movements.
Antenatal visits can seem very stressful and time-consuming. However, it is still in the best interest for you and your baby. To get the best out of your visit, be sure to write down beforehand questions or concerns you have. Always ask questions and make notes of the responses your doctor gives you.

Good luck!