Your baby’s heart is fully functional by the 16th week of pregnancy. This means that it has completely formed its various parts and is able to carry out its unique function of pumping blood. At this point, the normal fetal heart rate ranges from 110-160 bpm(beats per minute).
However, this may not always be the case.
During pregnancy, it’s super important to closely monitor the fetal heart rate and rhythm in order to quickly detect any abnormalities. If they do occur, an abnormal change in the heart rate and rhythm of a fetus’ heart is termed fetal arrhythmia.
In this article, you’d discover all you need to know about fetal tachyarrhythmia, an important heart condition in growing babies. You’d also learn how doctors monitor a baby’s heart rate.
Don’t Stop Reading.

What Exactly Is Fetal Tachyarrhythmia?
In plain terms, fetal tachyarrhythmia is a sustained heart rate that is higher than normal (higher than 160bpm). Generally, this heart rate is too fast for a baby. You might want to see fetal bradyarrhythmia too.
Fetal tachyarrhythmia is divided into:
- Mild Fetal Tachyarrhythmia: a sustained fetal heartbeat that ranges between 161-180 bpm.
- Fetal Tachyarrhythmia: a sustained fetal heartbeat that is above 180bpm.
How Can I Know My Baby’s Heart Rate?
There are two major ways to monitor a baby’s heartbeat. These include:
1. External Fetal Heart Monitoring
This involves the use of an ultrasound listening device to listen to and record your baby’s heartbeat. As expected, It is commonly done during routine antenatal clinics.
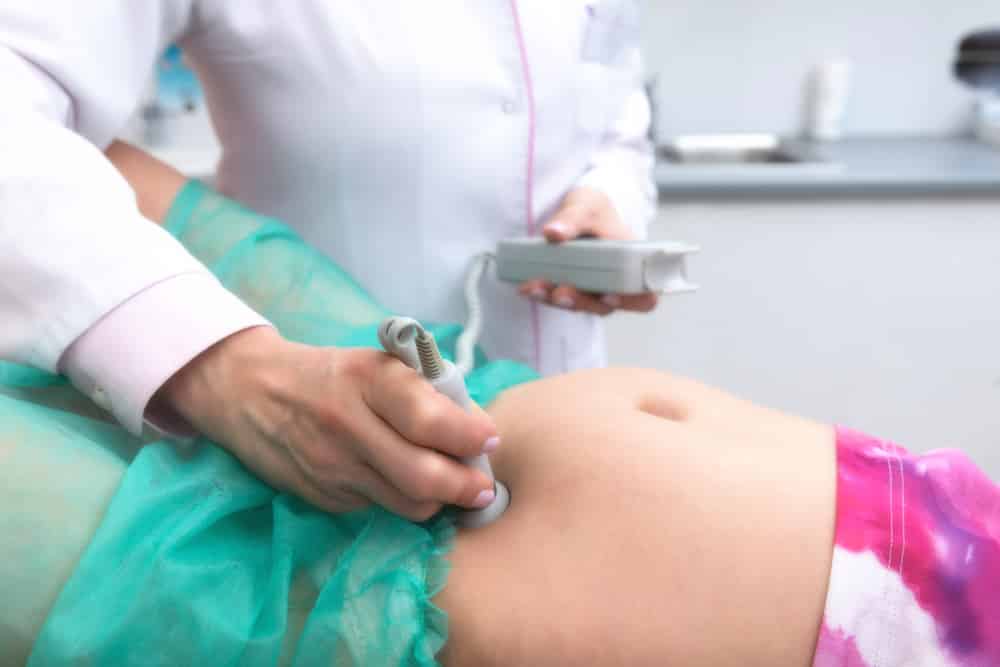
2. Internal Fetal Heart Monitoring
This method involves the use of a thin wire connected to your baby’s scalp through the cervix. Although this method gives more accurate readings, it is often uncomfortable for the mother.
How Does My Baby’s Heart Beat?
A baby’s heart, like an adult’s, beats by a series of electrical activities which spread throughout the walls of the heart. These electrical signals are generated from the sino-atrial(SA) node, which functions as the natural pacemaker of the heart.
The SA node is called the pacemaker because it sets the rate and rhythm of the heartbeat.
Generated impulses are conducted from the SA node to the chambers of the heart (atria and ventricles). Contraction of the atria and ventricles in response to transmitted electrical impulses is what results in a heartbeat.
As we mentioned earlier, tachyarrhythmia occurs when the heartbeat process occurs a lot faster than it should.
What Causes Fetal Tachyarrhythmia?
Generally, arrhythmias are caused due to problems with the heart’s conducting system. However, medical research shows certain conditions that are associated with fetal tachyarrhythmia.
Experts group these potential causes into maternal and fetal causes:
1. Maternal Causes
A persistently high fetal rate may be due to problems arising from the mother just as some cases of neonatal herpes. These include:
- Maternal fever
- High blood pressure
- Maternal ketosis
- Medications such as anti-cholinergic medications (e.g Benadryl)
- Substance abuse
2. Fetal Causes
In other instances, fetal tachyarrhythmia may result from problems in the fetus. These problems include:
- Fetal anaemia
- Prolonged fetal movement
- Congenital heart defects
- Chronic fetal hypoxia (low oxygen)
- Chromosomal anomalies

Types of Fetal Tachyarrhythmia
The most common forms of fetal tachyarrhythmia are generally classified into four types. From mild to severe, the types include:
1. Sinus tachyarrhythmia
In this case, there is normal conduction of signals from the atria to the ventricles. However, the heart rate is higher than normal (more than 180bpm but usually less than 200bpm). Most times, sinus tachyarrhythmia is temporary and is due to increased fetal activity.
In other cases, it may persist due to any of the underlying maternal or fetal conditions mentioned earlier.
2. Supra-ventricular tachyarrhythmia (SVT)
This is the most common form of fetal arrhythmia.
Most times, this condition develops between the 24th and 32nd weeks of gestation. In this type of fetal arrhythmia, the upper chamber of the heart beats significantly faster than the lower chamber. Supraventricular tachyarrhythmia results from defects in the electrical conducting system (SA node) of the heart.
Sometimes, the fetal heart rate may even be as high as 200bpm.
3. Atrial flutter
This is often classified as a type of SVT. It is an abnormal heart rhythm that starts in the atria of the heart, causing the atria to beat a lot faster than the ventricles.
Thankfully, atrial flutter hardly persists in most developing babies.
4. Ventricular tachyarrhythmia (VT)
This is a rare form of fetal tachyarrhythmia in which the ventricles beat at a faster rate than the atria. Most times, ventricular tachyarrhythmia is associated with heart conditions like cardiomyopathy, complete heart block, and long QT syndrome.
Diagnosis of Fetal Tachyharrhythmia
Generally, fetal arrhythmias are detected during routine maternal antenatal check-ups.
During these sessions, the doctor listens to the fetal heart rate with an ultrasound machine. If the pattern of heart rate recorded suggests fetal tachyarrhythmia, he/she would perform a comprehensive examination.
The comprehensive exam evaluates fetal movement, tone, and amniotic fluid level.
What Are The Associated Risks?
Usually, abnormal heart rhythms have little or no effects on the fetus. However, in more serious cases, there are certain risks that accompany the condition.
As with all forms of fetal arrhythmia, the major risks of fetal tachyarrhythmia are the development of “hydrops fetalis” and intrauterine death.
Hydrops fetalis is a serious condition that presents with the abnormal build-up of fluid in two or more body areas of a fetus. The development of Hydrops fetalis often calls for inducement of labor and immediate delivery of the baby.
Treatment of Fetal Tachyarryhthmia
Mild cases of fetal tachyarrhythmia usually require no form of treatment or therapy. However, the fetal heart rate should be closely and regularly monitored until the condition has fully resolved.
For more serious cases of fetal tachyarrhythmia, the treatment plan includes:
- Medications given to the mother to lower heart rate.
- Emergency delivery in case of foetal distress.
- Less commonly, open heart surgery may be necessary to correct the cause of the abnormal heart beat.
Delivery
Emergency delivery of a baby with tachyarrhythmia is a delicate process. In fact, it should only occur in a tertiary hospital with health workers skilled in postnatal cardiac care. This is because the delivery and postnatal care of patients with this condition involve a team of special cardiologists, pediatricians, and nurse practitioners.
In most cases, especially when the baby is at risk, a cesarean section is the safest option.
Postnatal Treatment
Of course, the treatment requirement after birth differs based on each baby’s arrhythmia and underlying conditions.
In mild cases, the heart rate may normalize on its own without treatment. However, medications may be necessary to lower the heart rate. Furthermore, mothers with underlying health conditions should continue using their regular medications.
In Conclusion,
The best option is to closely monitor every child with tachyarrhythmia until the condition is fully resolved.
This is really important because proper monitoring and treatment may be the key to a healthy and successful life for babies with this condition.
Finally, it helps to remember that with the right group of specialists and medical care, most cases of fetal tachyarrhythmia have excellent outcomes.

